There are three types of diabetes (or its proper name Diabetes Mellitus): Type 1, Type 2 diabetes and gestational diabetes.
Each is different in terms of causes and sometimes treatment, but the end effects on the body are the same.
Each is a serious disease.
Here is some information about each type of diabetes and how they are all a little bit different.
Type 1 Diabetes
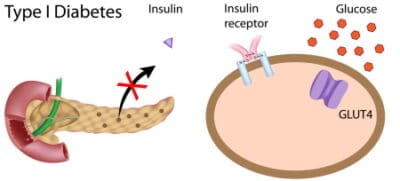
Diabetes type 1 used to be referred to as insulin-dependent diabetes. That term has been dropped, in part because some type two diabetics are insulin dependent as well.
This type of diabetes accounts for 10-15% of all people with this disease. Although it can appear at any age, it is commonly discovered in people under 40 years of age, hence the common reference to this type of diabetes as juvenile or juvenile onset diabetes.
Type 1 diabetes is an auto-immune disease. In a healthy body insulin is produced in the pancreas, and is used by the body for energy. If you have type one diabetes, glucose builds up in your blood instead of being used for energy.
This is because the pancreas does not produce insulin any longer. It is thought that the body’s defense system may attack insulin-making cells by mistake. Unfortunately, to this date research has not been able to determine why this happens.
Type I diabetes is thought to be triggered by environmental factors such as viruses, diet or chemicals in people genetically predisposed but again, no exact cause has been determined.
Those who have type one diabetes must inject themselves with insulin several times a day and follow a careful diet and exercise plan.
Type 2 Diabetes

What is type 2 diabetes? Previously known as non-insulin dependent or adult onset diabetes, it is the most common form of the disease, affecting 85-90% of all diabetics. This type of diabetes is on the rise in North America and around the world at an alarming rate.
Also known as late-onset diabetes, type two diabetes is characterized by insulin resistance and relative insulin deficiency. That means that insulin is still being produced by the body, sometimes in excessive amounts, but is not being taken up by the body’s cells for use as energy. Consequently there is often excess insulin floating around the body.
Type II diabetes has a genetic component, meaning that those whose family members have it are at a higher risk for developing it, but lifestyle factors are major risk factors for developing diabetes as well.
Excess weight, an improper diet containing a high amount of carbohydrates (especially simple carbohydrates found in things like white flour and sugar), a sedentary lifestyle, high levels of emotional stress and high blood pressure can all lead to the development of type 2 diabetes.
There are many health risks associated with being diabetic. For example, people with type II diabetes are twice as likely to suffer heart disease and cardiovascular problems.
Diabetic neuropathy can develop which develops from decreased blood circulation to the limbs and can result in the need for amputation of toes, feet or legs. Infections and blindness are other long term complications of poor diabetes management.
Type 2 diabetics need to make changes to their diets as part of their treatment. (See our information on diabetic cooking for suggestions on changes to make for a healthy diabetic diet). Exercise is also an essential part of managing diabetes.
Most people with diabetes type 2 are treated with prescription medication (like Metformin) that helps to make the body less resistant to the insulin it already produces. Some medications cause the body to produce more insulin, if it is thought that the patient is not producing enough. Some diabetics eventually require insulin injections several times daily to maintain their health.
The good news for those with this type of the disease is that proper diabetic nutrition, watching your weight, eating a healthy diet and making exercise a part of your daily life can prevent the need for insulin injections.
Gestational Diabetes
Gestational diabetes mellitus (often shortened to GDM) is a form of the disease that is diagnosed during pregnancy. It is a disease of carbohydrate intolerance that will often appear during pregnancy and disappear afterwards.
The risk factors for gestational diabetes include a family history of diabetes, maternal age (older mothers are at increased risk) and obesity. There are also ethnic groups with a high risk of developing type 2 diabetes.
While the carbohydrate intolerance that caused the diabetes often returns to normal after the birth, the mother is at a much higher risk for developing permanent diabetes later in life. As well, sometimes the diabetes does not abate and the mother is left with permanent type 2 diabetes immediately after the pregnancy.
Dietary changes during the pregnancy are a necessity. Often women will need prescription medication to manage the disease or may need to take insulin injections.
Managing Diabetes
Here are some tips from the Canadian Diabetes Association for managing your diabetes and maintaining your overall health and wellness – today and in the future:
- Take your insulin and/or other medications according to the regimen prescribed by your doctor
- Check your blood glucose levels regularly. Do what you can to keep them within your target range
- Follow a balanced diabetic diet plan
- Be or become physically active
- Keep your cholesterol and other blood fats in a healthy target range
- Maintain a healthy weight
- Keep your blood pressure at or close to the target level set with your doctor
- Manage stress effectively (Try exercising or meditation to get rid of stress)
- Take care of your feet and check them on a regular basis
- Don’t smoke
- Visit your dentist and eye care professional every year. Diabetics need a fully dilated eye exam once per year for prevention of complications.
- Visit your doctor on a regular basis and follow his/her recommendations, especially in terms of taking your medications as prescribed.
Look through the other pages on this site with information for diabetics. Being “armed” with the right information is the best way to prevent or manage this disease.
Diabetic cooking tips for those with type 1, type 2 diabetes and gestational diabetes.
You will find lots of diabetic recipes and suggestions here.
Please Note: Before adjusting your diet in any way, please consult your own medical practitioner. The opinions expressed on this site are not meant to constitute medical advice or take the place of your medical practitioner.
Sign up here and be the first to get new recipes and tips.
I would really appreciate it if you mention Cookingnook.com on your favorite social media sites. Thanks.











